Age-related brain diseases, including dementia, stroke, and late-life depression, present significant health challenges as our population ages. Recent research conducted by experts at Mass General Brigham has uncovered 17 modifiable risk factors that can lower the likelihood of developing these debilitating conditions. By addressing issues such as high blood pressure, poor diet, and lack of physical activity, individuals can actively engage in preventing dementia and improve overall brain health. Furthermore, understanding and modifying these risk factors not only enhances quality of life but also reduces the burden of these interconnected diseases. With an emphasis on lifestyle changes, this study highlights the importance of awareness and proactive measures for safeguarding cognitive longevity and wellbeing.
Collectively referred to as cognitive decline syndromes, age-related brain diseases encompass a range of disorders, including Alzheimer’s disease, cerebrovascular accidents, and severe geriatric mood disorders. The intersection of these conditions points to shared vulnerabilities, allowing for a more holistic approach to treatment and prevention. By identifying key lifestyle modifications that influence these ailments, health professionals can focus on strategies aimed at reducing stroke risk factors and improving mental health in older adults. This broad framework not only fosters improved brain function but also promotes an enriched, purposeful life as we age. Establishing connections among these health issues encourages a comprehensive understanding of the aging brain’s resilience against adversities.
Understanding Age-Related Brain Diseases
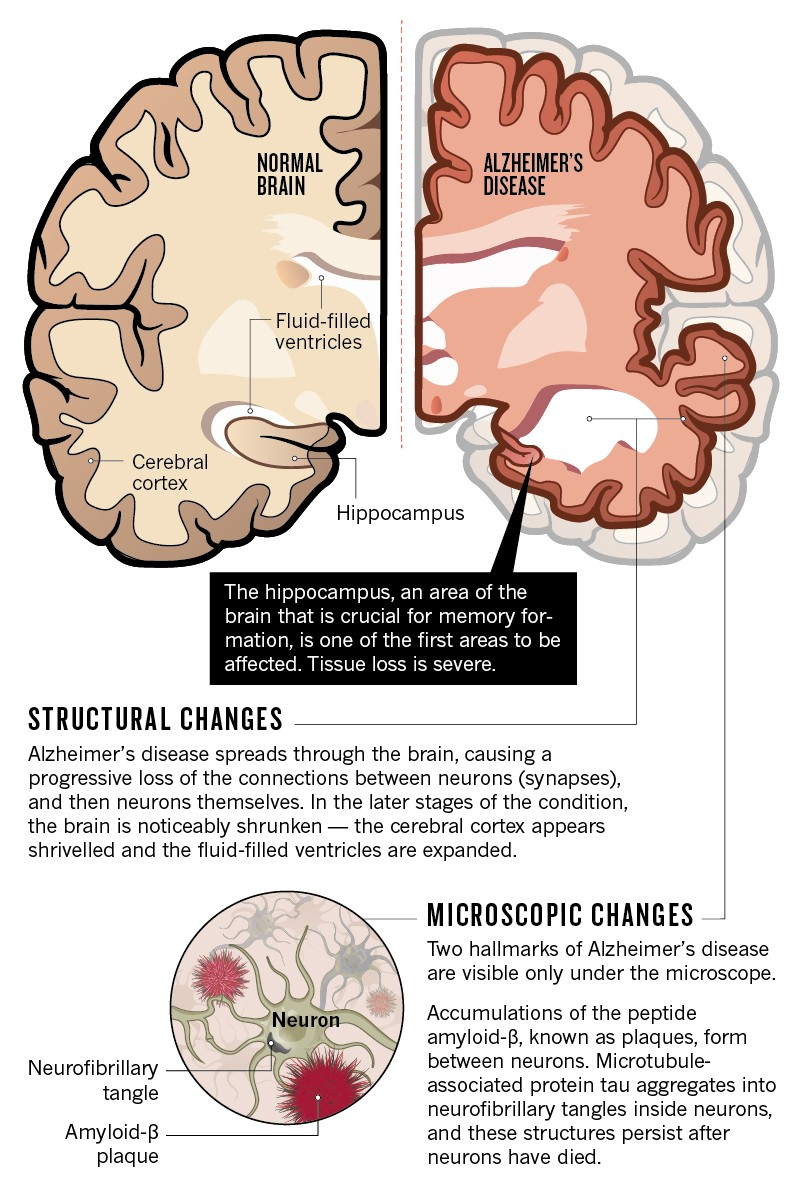
Age-related brain diseases encompass a range of conditions that typically manifest as individuals advance in age, including dementia, stroke, and late-life depression. These diseases share common risk factors that can impact cognitive functioning and overall mental health significantly. For instance, the interrelationships between these conditions highlight the importance of early interventions and adopting lifestyle modifications that can hinder their development. Learning about these diseases enables us to take proactive steps towards better brain health as we age.
Research has shown that addressing issues such as hypertension, diabetes, and obesity can drastically reduce the risk of developing these conditions. By understanding the underlying mechanisms that contribute to age-related brain diseases, health professionals can devise comprehensive strategies aimed at prevention. Engaging in discussions about these diseases lays the groundwork for raising awareness and fostering early detection, which is crucial for effective management and improving quality of life in older adults.
The Importance of Modifiable Risk Factors
Modifiable risk factors play a crucial role in preventing age-related brain diseases. They are conditions or behaviors that can be changed or improved through lifestyle choices. These include blood pressure management, dietary adjustments, physical activity, and smoking cessation. Notably, tackling these modifiable risk factors can yield significant benefits not only for brain health but for overall well-being. For instance, lowering high blood pressure can reduce the risk of stroke, while a balanced diet may lower the chances of developing dementia.
Furthermore, the study highlights that interventions aimed at modifying these risk factors can have cascading effects on reducing the prevalence of conditions like stroke and late-life depression. By focusing on manageable aspects of health, individuals can take charge of their brain health, leading to a better quality of life in later years. This proactive approach empowers individuals by offering clear and achievable steps towards reducing their risks of developing serious age-related brain diseases.
Preventing Dementia and Stroke through Lifestyle Changes
Preventing dementia and stroke is not solely about genetics; lifestyle plays a pivotal role. Engaging in regular physical activity, consuming a nutrient-rich diet, and managing chronic conditions like diabetes are essential steps towards safeguarding brain health. Research indicates that individuals who maintain an active lifestyle and engage in challenging cognitive activities may experience lower risks of cognitive decline. Simple changes, such as participating in community sports or dedicating time to mental exercises, can significantly influence long-term well-being.
Moreover, social engagement can further help mitigate risks associated with dementia and stroke. Connecting with others boosts mental health, exercise helps maintain physical fitness, and participating in meaningful activities fosters a sense of purpose. The interweaving of these lifestyle choices reinforces the importance of a holistic approach to health, ultimately leading to diminished risks of age-related brain diseases. Emphasizing social connections and cognitive engagement as everyday practices opens avenues for broader prevention strategies.
The Impact of Late-Life Depression on Brain Health
Late-life depression is often intertwined with age-related brain diseases, compounding the challenges faced by older adults. Studies show that untreated depression can elevate the risk of developing additional cognitive impairments, such as dementia. The emotional toll of depression may lead to decreased physical activity and poorer lifestyle choices, thus creating a negative feedback loop that exacerbates the symptoms of both depression and cognitive decline.
Addressing late-life depression requires clinicians to adopt a multidisciplinary approach that combines mental health support with strategies for improving physical health. Interventions focusing on lifestyle modifications and community engagement can not only improve mental health outcomes but also decrease the incidence of other brain diseases. With growing evidence supporting the connection between mental health and cognitive functioning, addressing late-life depression should be a cornerstone of comprehensive brain health strategies.
The Role of Social Engagement in Brain Health
Social engagement plays a vital role in maintaining cognitive function as we age. Interacting with peers and participating in community activities can stimulate the mind, reduce feelings of loneliness, and enhance overall emotional well-being. The beneficial effects of socialization extend beyond simple companionship; they can actively promote healthier brain functioning and lower the risks associated with age-related diseases.
Creating environments that foster social interactions can be as vital as physical exercise and diet in promoting brain health. Community groups, clubs, and volunteer opportunities not only provide social support but also encourage older adults to remain mentally active, which is crucial for sustaining cognitive health. By prioritizing social engagement as part of a holistic approach to health, individuals can cultivate lifestyles that significantly diminish their risk of dementia and related conditions.
Managing Stress to Improve Brain Function
Chronic stress has been identified as a significant risk factor for developing age-related brain diseases such as dementia and depression. Prolonged exposure to stress adversely affects mental and physical health, leading to inflammation and cognitive decline. Strategies to manage stress through mindfulness practices, regular physical activity, and social support systems can significantly mitigate these risks. As individuals learn to effectively cope with stress, they are better equipped to protect their cognitive health.
Incorporating stress-reduction techniques into daily routines, such as meditation or yoga, can enhance emotional resilience and improve overall brain health. These practices foster clarity of mind and promote healthier lifestyles, which are integral for combating the effects of stress. Understanding and managing stress can serve as a crucial component in the fight against age-related brain diseases, paving the way for improved cognitive longevity and quality of life.
The Connection Between Diet and Brain Health
Nutrition is one of the most powerful modifiable risk factors influencing brain health. A balanced diet rich in fruits, vegetables, lean proteins, and healthy fats provides the essential nutrients needed for optimal cognitive function. Conversely, a diet high in processed foods and sugars may contribute to the risk factors associated with age-related brain diseases, such as stroke and dementia. Research suggests that dietary patterns can significantly influence mood, cognition, and overall brain health.
Additionally, incorporating foods known for their brain-boosting properties can enhance cognitive functions and reduce the risk of decline. Foods like fatty fish, nuts, and leafy greens contain omega-3 fatty acids and antioxidants that protect against cognitive deterioration. As more evidence emerges regarding the intricate relationship between diet and brain health, individuals are encouraged to prioritize nutritious meals that support lifelong cognitive vitality.
Physical Activity: A Cornerstone of Brain Health
Physical activity emerges as a cornerstone of preventative strategies for aging populations concerned with brain health. Engaging in regular exercise not only benefits physical well-being but also boosts cognitive functions and reduces the risk of developing age-related brain diseases. Studies consistently demonstrate that individuals who remain physically active are less likely to experience cognitive decline, depression, and other neurological diseases.
Moderate aerobic activities, tailored strength training, and even simple daily movements can contribute significantly to maintaining brain and overall health. Furthermore, integrating physical activity into social settings enhances motivation and accountability, facilitating a more holistic approach to wellness. As healthcare begins to emphasize prevention over treatment, the incorporation of regular physical activity remains essential for reducing risks associated with age-related brain diseases.
Understanding the Brain Care Score
The Brain Care Score represents a groundbreaking tool aimed at assessing and enhancing brain health by evaluating multiple risk factors associated with age-related brain diseases. Developed by researchers at Mass General Brigham, it utilizes data collected from various studies to provide a comprehensive overview of individual brain health. By quantifying risk factors such as cholesterol levels, hypertension, and lifestyle habits, the Brain Care Score helps guide people in making informed decisions about their brain health.
Regular use of the Brain Care Score can facilitate early detection of potential problems, allowing individuals and healthcare providers to create personalized prevention plans. This evidence-based approach not only empowers individuals to take proactive measures in improving their health but also stresses the importance of lifestyle changes that can mitigate the risk of dementia, stroke, and depression. As public awareness of the Brain Care Score increases, it paves the way for a more focused dialogue on brain health and disease prevention.
Frequently Asked Questions
What are the modifiable risk factors associated with age-related brain diseases?
Modifiable risk factors for age-related brain diseases, including stroke, dementia, and late-life depression, consist of various health and lifestyle choices that can be changed. Key factors include high blood pressure, kidney disease, diabetes, poor diet, physical inactivity, excessive alcohol consumption, smoking, and chronic stress among others. By addressing these risks through behavior modification, individuals can potentially lower their chances of developing these conditions.
How can preventing dementia be achieved through lifestyle changes?
Preventing dementia can be effectively achieved by making lifestyle changes that target shared risk factors. Engaging in regular physical activity, maintaining a healthy diet, managing stress levels, ensuring adequate sleep, and preventing obesity are crucial. Moreover, staying socially engaged and treating conditions like high blood pressure and diabetes can further help reduce the risk of dementia, as they are significant modifiable risk factors.
What is the significance of social engagement in preventing late-life depression?
Social engagement is a vital modifiable risk factor in preventing late-life depression. Positive social interactions and relationships contribute to emotional well-being and can significantly mitigate feelings of loneliness and isolation. By staying connected with friends and family and participating in community activities, older adults can improve their mental health and decrease their chances of developing depression.
Are stroke risk factors similar to those for dementia and late-life depression?
Yes, many stroke risk factors overlap with those for dementia and late-life depression. Common factors include high blood pressure, diabetes, obesity, smoking, and physical inactivity. Addressing these shared risk factors through lifestyle modifications, such as adopting a healthier diet and increasing physical activity, can reduce the risk of all three conditions, highlighting the interconnected nature of age-related brain diseases.
How does chronic stress relate to age-related brain diseases?
Chronic stress is linked to a higher risk of age-related brain diseases such as stroke, dementia, and late-life depression. Persistent stress can lead to hormonal changes and inflammation that adversely affect brain health. Managing stress through relaxation techniques, physical activity, and social support can be an effective approach in lowering the risk of developing these conditions.
What role does physical activity play in maintaining brain health?
Physical activity plays a crucial role in maintaining brain health and can significantly lower the risk of age-related brain diseases. Regular exercise helps manage blood pressure, reduces the risk of obesity, and improves overall physical and mental health. Engaging in both aerobic and cognitive activities can enhance brain function and decrease the likelihood of developing stroke, dementia, and depression.
Can diet influence the risk of age-related brain diseases?
Absolutely, diet has a profound influence on the risk of age-related brain diseases. A poor diet high in saturated fats, sugars, and processed foods can increase the risk of obesity, diabetes, and cholesterol-related issues, which are all modifiable risk factors for stroke, dementia, and late-life depression. Conversely, a balanced diet rich in fruits, vegetables, whole grains, and healthy fats supports brain health and reduces these risks.
What is the Brain Care Score and how does it relate to preventing age-related brain diseases?
The Brain Care Score is a tool developed by Mass General Brigham researchers to assess efforts aimed at protecting brain health. It incorporates various modifiable risk factors associated with age-related brain diseases such as stroke, dementia, and late-life depression. By using the Brain Care Score, individuals can identify areas for improvement in their health behaviors, potentially reducing their risk of developing these interconnected conditions.
How important is sleep quality in preventing dementia and late-life depression?
Sleep quality is extremely important in preventing dementia and late-life depression. Poor sleep can exacerbate symptoms of depression and cognitive decline. Ensuring that you get adequate, restful sleep each night can improve mood, cognitive functioning, and overall brain health, thereby acting as a modifiable risk factor that can diminish the risk of these age-related brain diseases.
What types of activities can help reduce the risk of age-related brain diseases?
Engaging in a variety of activities can significantly reduce the risk of age-related brain diseases. This includes regular physical exercise, cognitive activities like puzzles and reading, maintaining social connections, and participating in community services. These actions help foster brain health and can effectively lower the risk of conditions such as stroke, dementia, and late-life depression.
| Risk Factor | Description |
|---|---|
| Diabetes | Risk factor for stroke, dementia, and depression. |
| Blood Pressure | High blood pressure is a major risk factor for all three conditions. |
| Kidney Disease | Increases the risk of stroke, dementia, and depression. |
| Fasting Plasma Glucose | High blood sugar levels are a risk factor. |
| Total Cholesterol | High cholesterol levels can increase risk of stroke and dementia. |
| Alcohol Use | Excessive consumption linked to higher risk of all three conditions. |
| Diet | Poor dietary choices contribute to development of conditions. |
| Hearing Loss | Linked as a modifiable risk factor for dementia. |
| Pain | Chronic pain can increase risk of depression and other conditions. |
| Physical Activity | Lack of activity is a risk factor for all three conditions. |
| Purpose in Life | Lack of purpose can lead to depression and other disorders. |
| Sleep | Poor sleep quality increases risk of depression and associated issues. |
| Smoking | Significant risk factor for stroke, dementia, and depression. |
| Social Engagement | Lack of social interaction can contribute to depression and other conditions. |
| Stress | Chronic stress can increase risk of depression. |
| Obesity | A risk factor for stroke, dementia, and depression. |
Summary
Age-related brain diseases are significantly influenced by a variety of modifiable risk factors. This study highlights the importance of addressing these factors, such as high blood pressure, kidney health, and lifestyle choices like diet and exercise, to mitigate the risk of stroke, dementia, and late-life depression. By understanding and adjusting these factors, we can take substantial steps toward reducing the prevalence of these debilitating conditions and enhance overall brain health.